The following checklist is a useful tool to use when you develop a management plan with your health care team. Later modules will provide more detail about all of the important steps that might be included in your management plan.
Click here to download the COPD-X checklist in PDF format.
 C: Confirm Diagnosis
C: Confirm Diagnosis
By now your doctor will have informed you that you have COPD.
To confirm your diagnosis and to assess the severity of your COPD it is important that you have a breathing test performed (called spirometry). You should also have your spirometry checked regularly to monitor the progress of your COPD.
You may have this done at the GP’s or specialist clinic, in a lung function laboratory or with another member of your health care team.
- I have had a Spirometry breathing test
 O: Optimise Function
O: Optimise Function
To improve your condition your doctor will prescribe treatments.
These treatments may include inhaled medicines (puffers), exercises or ‘Pulmonary Rehabilitation’ and treatments for other common medical conditions that frequently complicate COPD e.g. osteoporosis.
It is very important that you use your medicines correctly and as prescribed and actively participate in a supervised exercise program.
- I understand my medicines and what each is doing for me
- I have had my inhaler technique assessed (regularly) and learnt how and when to use my medicines properly
- I have been referred to a Pulmonary Rehabilitation group
- I regularly exercise
- I have discussed my other medical problems with my doctor and other members of the COPD team
- I have had regular health checks with my doctor to monitor my signs and symptoms
 P: Prevent Deterioration
P: Prevent Deterioration
COPD is a progressive disease, however, there are a number of things you can do to prevent your COPD from getting worse.
The most important of these is to stop smoking if you have not already done so. In addition to this you should have a basic understanding of what your blood oxygen levels are and ensure you get yearly immunisations against the influenza ‘flu’ virus.
- I have successfully stopped smoking
If you are a current smoker:
- I have discussed stopping with a member of my COPD team
- I know how to start a quit plan
- I am aware of the medicines that can help me stop smokingI have had my yearly flu immunisation
- I have had my pneumococcal immunisation
- I have had my blood oxygen level checked
- I know what my blood oxygen level is
 D: Develop Support Network and Self-Management Plan
D: Develop Support Network and Self-Management Plan
Self-management support is the provision of education and supportive interventions by health care staff to assist you in increasing your skills and confidence in managing your COPD. Members of the health care team including your specialist GP, nurse, physiotherapist or pharmacist are there to help you become a good self-manager.
- I feel that I can ask questions about my health care
- My health care team and I have developed a written management plan to assist me in managing my health better
- I have talked about an advanced health care directive with my doctor. (Advanced Health Care Directives are addressed in Module 5).
 X: Manage Exacerbations (Flare Ups)
X: Manage Exacerbations (Flare Ups)
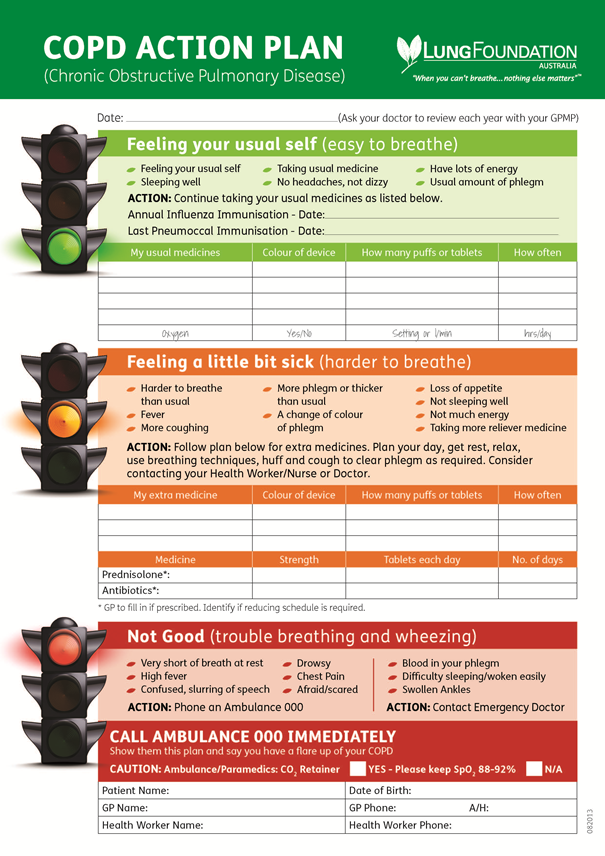
All people with COPD are at risk of exacerbations or ‘flare ups’ of their condition. A very important goal of your COPD management is to prevent flare ups or if they do occur treat them early to prevent them from getting worse. A written COPD Action Plan can help you identify flare ups and provides you with instructions about how to manage them at an early stage of worsening illness.
- My doctor and I have developed a written COPD Action Plan
- I am aware of the signs and symptoms of a flare up
- I know how to increase my treatment during a flare up
- I have medicine or prescriptions at home to start my action plan
- I know how long to increase my treatment during a flare up
- I know when to call for assistance (ambulance or hospital)
 C: Confirm Diagnosis
C: Confirm Diagnosis
 O: Optimise Function
O: Optimise Function P: Prevent Deterioration
P: Prevent Deterioration  D: Develop Support Network and Self-Management Plan
D: Develop Support Network and Self-Management Plan X: Manage Exacerbations (Flare Ups)
X: Manage Exacerbations (Flare Ups)